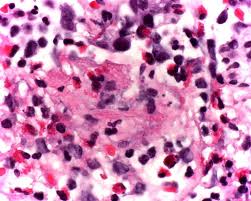
 Three days after discharge, he was readmitted because of increased coughing. His temperature was 38.2°C, the heart rate, 128/minute; and the respiratory rate, 32/minute. A chest roentgenogram demonstrated worsened diffuse interstitial infiltrates. The BAL was repeated, and an open lung biopsy performed. Microscopic examination of the BAL fluid demonstrated septate branching hyphae consistent with Aspergillus sp. Numerous palisading granulomas with necrotic centers containing eosinophils, neutrophils, and hyphae were seen microscopically in the open lung biopsy (Fig 2). Amphotericin B was given intravenously. Aspergillus fumigatus was cultured from both BAL fluid and lung. Pseudomonas cepacia was cultured from the lung, and from a blood specimen taken two days after readmission; ticarcillin and tobramycin were administered.
Three days after discharge, he was readmitted because of increased coughing. His temperature was 38.2°C, the heart rate, 128/minute; and the respiratory rate, 32/minute. A chest roentgenogram demonstrated worsened diffuse interstitial infiltrates. The BAL was repeated, and an open lung biopsy performed. Microscopic examination of the BAL fluid demonstrated septate branching hyphae consistent with Aspergillus sp. Numerous palisading granulomas with necrotic centers containing eosinophils, neutrophils, and hyphae were seen microscopically in the open lung biopsy (Fig 2). Amphotericin B was given intravenously. Aspergillus fumigatus was cultured from both BAL fluid and lung. Pseudomonas cepacia was cultured from the lung, and from a blood specimen taken two days after readmission; ticarcillin and tobramycin were administered.
Precipitating antibodies to Aspergillus sp were reported from serum sent to the other laboratory during the first admission. A nitroblue tetrazolium test was normal. Respiratory failure ensued, and despite mechanical ventilation and inotropic support, the patient died the following day. At autopsy, the lungs were grossly consolidated. There were nearly confluent granulomas containing fungal hyphae, and parenchymal destruction with vascular invasion was seen. Although the thymus, spleen, and lymph nodes were depleted, appropriate T-and B-cell areas were represented. White blood cell function studies were done on the patient’s mother and were normal. Aspergillus fumigatus grew from a culture of the compost pile.
Category: Pulmonary disease
Tags: aspergillosis, eosinophilic pneumonia, lung biopsy, pneumonia
© 2011 - 2024 buy-asthma-inhalers-online.com. All rights reserved.