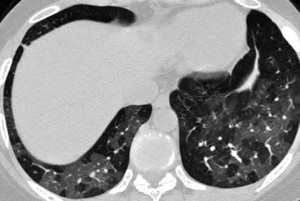
 Systemic sclerosis or scleroderma is a generalized connective tissue disorder of unknown origin that commonly affects the lungs, leading to fibrosis of the alveolar walls and narrowing of the pulmonary arterial tree. A restrictive pattern of abnormality with reduced lung volumes, as well as a diffusion impairment, are the cardinal features of pulmonary function in systemic sclerosis. Obstructive changes such as atrophy and fibrosis of the muscular and elastic layers of the bronchi and peribronchial fibrosis have also been found at autopsy in patients with scleroderma.
Systemic sclerosis or scleroderma is a generalized connective tissue disorder of unknown origin that commonly affects the lungs, leading to fibrosis of the alveolar walls and narrowing of the pulmonary arterial tree. A restrictive pattern of abnormality with reduced lung volumes, as well as a diffusion impairment, are the cardinal features of pulmonary function in systemic sclerosis. Obstructive changes such as atrophy and fibrosis of the muscular and elastic layers of the bronchi and peribronchial fibrosis have also been found at autopsy in patients with scleroderma.
Although there is agreement that the large airways are not commonly affected, the exact frequency and importance of small airways dysfunction (SAD) in systemic sclerosis still awaits confirmation. Gutadau-ria et al suggested that there is a high prevalence of dysfunction, with the small peripheral airways probably being the initial site of lung involvement and several other authors agree with this concept. On the other hand, cigarette smoking has been considered as the leading pathogenetic factor resulting in airways obstruction in scleroderma patients with pulmonary involvement. These authors suggested that SAD might be due to the effect of concomitant cigarette smoking rather than to the underlying disease.
The present study was designed to evaluate pulmonary function, focusing on the presence of SAD, in a “pure” population of nonsmoking patients with systemic sclerosis. An age- and sex-matched group of nonsmoking control subjects was studied in parallel.
Category: Pulmonary disease
Tags: pulmonary function, pulmonary involvement, scleroderma, systemic sclerosis
© 2011 - 2024 buy-asthma-inhalers-online.com. All rights reserved.